Former Atlanta TV news reporter Melissa Stern first felt a lump in her right breast around August 2019. Family members all confirmed that it was something she should have checked out, so she made an appointment with the gynecologist she was seeing prior to beginning care at Emory Healthcare. The doctor told her that since she was so young and had no family history, it was “probably nothing.”
The lump still hadn’t gone away several months later. “It was bothering me, and I’m very in tune with my body,” says Melissa. “So I went and got it checked out.” She proactively went for a mammogram and ultrasound. Everything “came back abnormal,” Melissa says. The radiologist asked how old she was—she was about to turn 31—and recommended she get a biopsy.
Early detection of breast cancer can save lives. When Melissa discovered a new lump, consulting her health care provider was the right step for her to take. Typically, patients like Melissa would then be referred for a diagnostic mammogram, which is used to check for breast cancer after a lump or other sign or symptom has been found. Most of the time, these suspicious areas don’t turn out to be cancer, but the only way to know for sure is through follow-up tests. You can read more about how breast cancer is diagnosed at Emory Breast Imaging Center at winshipcancer.emory.edu.
On February 26, 2020, after having the biopsy, Melissa got a phone call no one ever wants to receive. “I’ll never forget,” she says. They told her, “You have invasive ductal carcinoma.” The cancer was stage 2, which means that the tumor in the breast measures 2 to 5 centimeters in diameter or cancerous cells have spread to the lymph nodes in the underarm area.
Stage 2 breast cancers are curable with a combination of treatments, which in Melissa’s case consisted of surgery, local and systemic chemotherapy, radiation therapy and hormonal therapy. Breast cancer is the most common cancer in women in the United States, except for skin cancers, accounting for about 30% (or 1 in 3) of all new female cancers each year. The American Cancer Society estimates that in 2023, about 297,790 new cases of invasive breast cancer will be diagnosed in women—including about 55,720 new cases of ductal carcinoma in situ (DCIS). About 43,700 women will die this year from breast cancer. However, the five-year survival rate for stage 2 breast cancer is 93% for women who have completed treatment.
 Melissa waited about a month to begin chemotherapy because she “had a million things to do,” including going to a lot of doctor’s appointments, filling out forms and freezing her eggs to ensure that she and her then-boyfriend, Jordan, could eventually have the children they wanted.
Melissa waited about a month to begin chemotherapy because she “had a million things to do,” including going to a lot of doctor’s appointments, filling out forms and freezing her eggs to ensure that she and her then-boyfriend, Jordan, could eventually have the children they wanted.
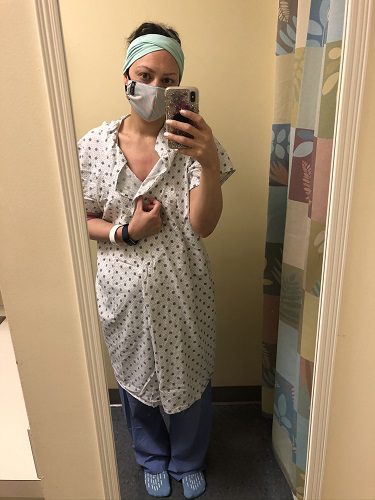
When she went to Winship Cancer Institute of Emory University for her first infusion on March 31, 2020, early in the COVID-19 pandemic, people were starting to wear face masks and hospitals were forced to restrict visitors. This meant, says Melissa, “I had to start going to these appointments, and going through all of this stuff that was unknown to me, by myself.”
Melissa’s family was as supportive as they could be from Florida while she was in Atlanta. Because of COVID-19 precautions, her physician father said they would put her at more risk by coming to see her than by supporting her from afar. Fortunately, the hospital visitor policy did allow people undergoing chemotherapy to have one guest. So Jordan was allowed to accompany her, but only for her infusions. For all the other appointments—such as when she was freezing her eggs or undergoing radiation—nobody was allowed to go with her. “I had a double mastectomy,” says Melissa, “and I had to go in by myself.”
Why Winship?
Melissa recalls that when she was first diagnosed, her parents asked her if she wanted to consider seeking treatment in New York City, Houston or other places. Melissa responded, “I live in Atlanta, Emory’s here, Winship is here. Why would I go to another state to get treatment when I could go to one of the best hospitals in the country? I mean, people fly around the country to come here.”
Melissa’s friends and medical professionals from around the country, who didn’t know one another, all recommended the same doctor—Winship breast oncologist Jane Lowe Meisel, MD. “She’s been amazing,” says Melissa. “I really don’t think I could have gone through everything I’ve gone through without her.”
Melissa saw for herself what draws people to Winship in her very first infusion session when she experienced a negative reaction to the first medication she received, which was used to prevent nausea. “All of a sudden I can’t breathe and I’m calling for Jordan,” Melissa recalls. “In a matter of seconds, I think there were like 10 doctors and nurses around me.” She warmly praises her nurses and others at Winship. “You just form this bond with them, and they’re just amazing people,” she says.
The care and expertise at Winship impressed Jordan, too. “Seeing Dr. Meisel made me feel like Melissa was in good hands,” he says. “We definitely feel connected to Winship and the community. You can tell just walking around that the nurses and doctors all have an incredible relationship, and you feel like you’re walking into this community when you walk into the building.” He adds, “Everyone at Winship seems like they’re there for you. And whether they’re helping another 20 patients in the same room, it seems like whenever we needed something, they were already proactive and were on their way with it, or had already thought of it.”
Melissa and Jordan’s relationship made an impact on her care team as well. “It was a pleasure and a privilege to take care of Melissa,” says Dr. Meisel. “Seeing her get through chemotherapy, surgery, and radiation with so much strength and grace was an inspiration for me and for our entire team.”
In Sickness and In Health
Jordan also helped tremendously. He and Melissa met while she was interviewing for a job in Atlanta, and they had been dating for a little over a year at the time of her diagnosis. “I remember calling him and telling him that I had cancer,” Melissa says. She wondered if it “would put an end to us.” She explains, “It’s a lot for a caregiver to deal with as a family member, a husband, a wife, a sibling—let alone a boyfriend.” She adds, “I remember he said, ‘We’re going to get through this together.’ And that’s when I knew for sure he was ‘the one.’”
For his part, Jordan says, “I knew in the back of my mind that we were going to be okay because Melissa is incredibly strong and passionate.” He was inspired by the example of his own grandmother, who’d had breast cancer, and is now in her early nineties “still alive and doing great.”
 The night before Melissa was going to start radiation, Jordan suggested they go out for dinner on the rooftop of Ponce City Market in Atlanta. He ushered her to the side where private events are held. Their song was playing and there were pictures and roses. “And then I got down on one knee and proposed,” Jordan recalls. “A lot of my speech in the proposal had to do with going through this journey with Melissa.”
The night before Melissa was going to start radiation, Jordan suggested they go out for dinner on the rooftop of Ponce City Market in Atlanta. He ushered her to the side where private events are held. Their song was playing and there were pictures and roses. “And then I got down on one knee and proposed,” Jordan recalls. “A lot of my speech in the proposal had to do with going through this journey with Melissa.”
Melissa and Jordan were married in March 2022, and Melissa is now pregnant with their daughter, due in June 2023.
Melissa says, “I always joke that we’ve got the ‘in sickness and in health’ part down.” Jordan adds of their experience with cancer, “Once we’ve conquered what we already have, we can do anything together.”
About Winship Cancer Institute of Emory University
Winship Cancer Institute of Emory University is Georgia’s only National Cancer Institute-designated Comprehensive Cancer Center, a prestigious distinction given to the top 3% of cancer centers nationwide for conducting cancer research and providing training that is transforming cancer care, prevention, detection and survivorship. Winship discovers, develops, delivers and teaches some of the world’s most effective ways to prevent, detect, diagnose and treat each patient’s unique cancer. Cancer care at Winship includes specialists with deep expertise and experience in cancer; multidisciplinary evaluation, treatment planning and care coordination that caters to each patient’s individual needs; therapies supported by the latest advances in cancer research; and comprehensive clinical trials and support services.



