Jerry Bullard thought he could manage his low back pain until sharp, stabbing sensations nearly brought him to a standstill on a 2019 vacation to Israel. The aching hurt so badly that he took pain medication — something he always tries to avoid — to ease the discomfort and make it through the trip.
“The pain in my legs was so bad, I could barely walk,” Jerry says. “When my wife and I returned home, the pain got worse. That’s when I contacted the doctors at the Emory Spine Center.”
Based on MRI scans, physicians diagnosed him with spinal stenosis, a condition where the space inside the backbone is so small that it puts pressure on the spinal cord and nerves. The result, for many people, is low back pain.
For Jerry, the chronic, overwhelming back pain sidelined his favorite activities. Painful bouncing on the tractor meant he could no longer mow the grass on his 11.5-acre property. Lifting a 60-pound tow-behind camper caused too much pain, so he and his wife gave up camping. They even made plans to move into a senior living community.
As depression over his condition set in, Jerry, a 72-year-old retired plumber, pursued many therapy options.
Multiple Treatment Failures
 Jerry’s original doctors, located in another hospital system, performed invasive back surgery at first. Although the pain initially subsided, he needed a second surgery about a year later. That procedure also failed.
Jerry’s original doctors, located in another hospital system, performed invasive back surgery at first. Although the pain initially subsided, he needed a second surgery about a year later. That procedure also failed.
“The second surgery didn’t help a bit. The pain intensified,” he says. “It would go up the right side of my back and into my hips. I was miserable, just miserable.”
A string of other treatment attempts followed these surgeries. Jerry attended physical therapy twice a week. But each session provided only an hour of pain relief. He also received four steroid injections. Unfortunately, each shot proved less effective than the previous one.
Doctors also suggested two options to trick the nerves into ignoring the pain. A TENS (transcutaneous electrical nerve stimulation) machine that delivered small electrical impulses via electrodes to relax back muscles, and dry needling—inserting thin acupuncture needles to relieve trigger points. Both failed.
“My doctors tried various things, but nothing worked,” Jerry says. “That’s when I listened to a friend who plays pickleball with my wife, and I called Emory Orthopaedics & Spine Center at Flowery Branch to make an appointment to talk about a peripheral nerve stimulator.” At Emory Healthcare, Jerry hoped to find a new, successful solution for his pain.
Peripheral Nerve Stimulator Success
In October 2022, Jerry and his wife sat down with Anand Joshi, MD, MHA, a physical medicine and rehabilitation specialist with the Emory Orthopaedics & Spine Center, to discuss how a SPRINT® peripheral nerve stimulator might offer some benefit. After many years of physical labor, Jerry experienced wear and degeneration in his spine that caused his pain. This device also aided in strengthening his back core muscles.
“We think a common reason people have back pain is that their core muscles are not as strong as they need to be,” Dr. Joshi says. “A peripheral nerve stimulator can help patients achieve strength above and beyond what a core strengthening program with a physical therapist can do.”
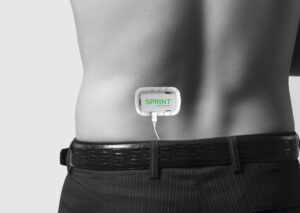 The process behind implanting this 60-day treatment is simple. The 45-minute, minimally invasive procedure uses a local anesthetic. Doctors insert a wire the size of a sewing thread two to three inches into the patient’s back using X-ray and ultrasound guidance. That wire rests within the core muscles that support the spine. Doctors then connect the other end of the wire to a remote control-powered transmitter worn outside the body. Patients send electrical impulses for six to 12 hours daily to prompt the core muscles to reduce the pain by contracting and strengthening.
The process behind implanting this 60-day treatment is simple. The 45-minute, minimally invasive procedure uses a local anesthetic. Doctors insert a wire the size of a sewing thread two to three inches into the patient’s back using X-ray and ultrasound guidance. That wire rests within the core muscles that support the spine. Doctors then connect the other end of the wire to a remote control-powered transmitter worn outside the body. Patients send electrical impulses for six to 12 hours daily to prompt the core muscles to reduce the pain by contracting and strengthening.
Unlike many treatments for low back pain, a peripheral nerve stimulator could help almost anyone with this chronic issue. Patients with pacemakers or metal implants from previous surgeries should talk with their doctors about whether it’s safe to use this device. Dr. Joshi says Jerry was a near-perfect candidate, mainly because all other treatment options had failed.
According to Jerry, the pain relief was nearly immediate. And he has remained largely pain-free even after removing the peripheral nerve stimulator. Several weeks post-procedure, Jerry says he’s still enjoying 75% pain relief.
“I had the procedure done, and the pain in my hips went away that day. It was that fast, and the pain that went up my right side eased up a lot,” he says. He’s recommended the procedure to others in his physical therapy group. “Since Dr. Joshi removed the stimulator, I’ve felt much better. My wife and I had cut out travel, exercise — everything. Now, I can get my chainsaw out to work in the yard, and I need to start going to the gym. It’s a miracle.”
Repeating the Procedure
With a peripheral nerve stimulator, roughly 60% of patients experience greater than 50% relief of pain at the one-year mark. Then, if the pain returns, a patient and their doctor can decide to repeat the procedure. The ultimate goal, Dr. Joshi says, is to make patients more comfortable.
“The whole idea behind this treatment is to — potentially and optimally — put patients in the position to have long-term pain relief,” he says. “For Jerry, he experienced both a reduction in his pain and an increase in his ability to function. So, his quality of life improved.”
Today, Jerry is back behind the wheel of his tractor. He and his wife have abandoned the idea of moving to a retirement community, and they’re planning more camping trips and a cruise down the Rhine River. And if the pain returns, Jerry’s not worried. He already knows what he’ll do.
“In the past two months, I have my life again. Even if I had no insurance and had to pay for the procedure out of pocket, I would do it again without hesitation,” he says. “It has changed my life.”
Visit the Emory Healthcare website to learn more about low back pain and the Emory Orthopaedics & Spine Center. We are dedicated to treating all your orthopaedic, spine and sports injuries.